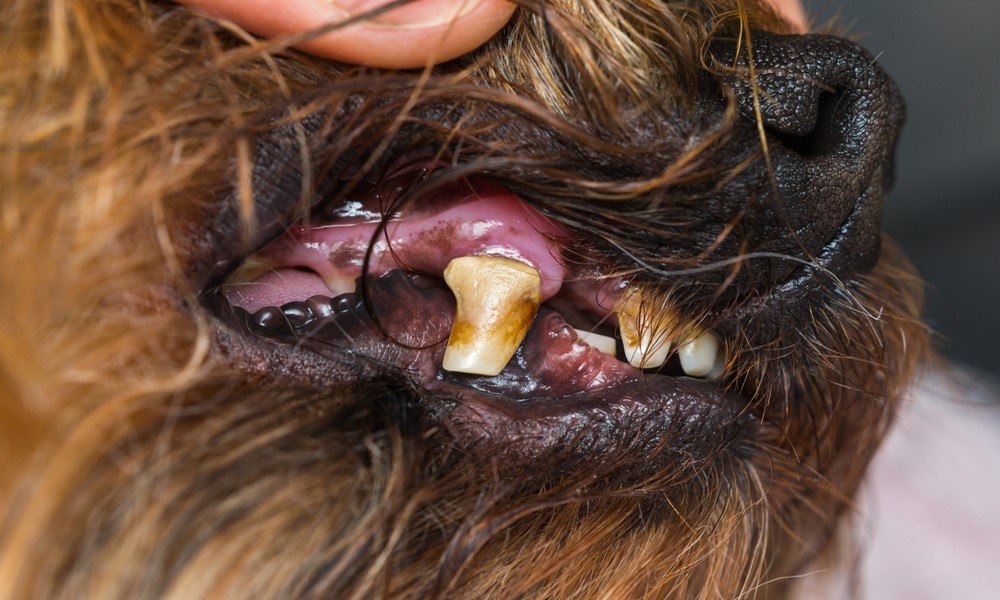
“Doggy breath” has been culturally normalized to the point that most owners barely register it, but the smell is a clinical sign. It indicates bacteria. Bacteria in the mouth of a dog, sustained over time, produce the single most common disease condition in adult small-animal medicine. The American Veterinary Medical Association estimates that about 80 percent of dogs show signs of periodontal disease by age three, and practices across the Twin Cities, Douglas Animal Hospital in Osseo among them, see the downstream consequences constantly: loose teeth, chronic pain, and jaw abscesses owners never connected to what was happening in the mouth.
Why “Dog Breath” Is Actually a Diagnosis
Plaque is a biofilm of bacteria and salivary proteins that forms on tooth surfaces within hours of eating. Saliva contains enough calcium that within roughly 48 hours, unbrushed plaque mineralizes into tartar. Tartar itself is not the problem. The problem is what happens underneath it, where bacteria work below the gumline, dissolve the ligaments that hold teeth in place, and eat through the bone that supports them.
The smell is the byproduct. Volatile sulfur compounds released by anaerobic bacteria living in periodontal pockets produce the specific odor that gets dismissed as normal. A healthy mouth does not smell.
The Signs Most Owners Miss
Dogs hide oral pain exceptionally well. A dog with a fractured molar or a severely infected tooth will usually keep eating until the tooth is visibly loose, which is why most periodontal disease gets caught late.
Earlier indicators are worth knowing. Reluctance to chew hard kibble, dropping food, chewing on one side of the mouth, blood on a favorite chew toy, pawing at the face, and red gum margins all indicate oral pain before a loose tooth makes the problem obvious. Small breeds and brachycephalic breeds are disproportionately affected because the teeth are crowded into jaws not designed for that dental formula, and tartar accumulates faster in the gaps.
The Stages of Periodontal Disease
The American Veterinary Dental College grades periodontal disease on a scale from zero to four.
Stage one is gingivitis, inflammation of the gum margin before any attachment has been lost. It is the only stage that is fully reversible. Stage two involves up to 25 percent attachment loss, which a radiograph will show even when the tooth still looks stable. Stage three reaches 25 to 50 percent. Stage four, at more than 50 percent, usually requires extraction. The distinction matters because most of the relevant information lives below the gumline, where it cannot be seen without dental radiographs.
Why Anesthesia-Free Cleanings Are Not a Shortcut
The option that keeps coming back in marketing is the “anesthesia-free” dental cleaning. The pitch sounds reasonable, but these services only remove the visible tartar above the gumline. They cannot probe periodontal pockets, cannot scale below the gumline where disease actually progresses, cannot take radiographs, and rely on restraining an alert dog while sharp instruments work near the teeth.
The American Veterinary Dental College and the American Animal Hospital Association are both explicit that these procedures are not a substitute for professional dentistry under anesthesia. A clean-looking mouth after an awake cleaning often hides disease that has already reached stage two or three.
What a Proper Dental Visit at Douglas Animal Hospital Actually Involves
A comprehensive oral health assessment and treatment (COHAT) is a more involved procedure than most owners realize. It starts with pre-anesthetic bloodwork to flag any risks. The dog is then placed under general anesthesia with intubation, which protects the airway from the aerosolized water and bacteria generated during scaling. Full-mouth dental radiographs come next, and they usually identify pathology the visible exam missed, including resorptive lesions, fractured roots, and abscessed premolars. Ultrasonic scaling above and below the gumline removes the disease-driving deposits. Each tooth is probed and charted, surfaces are polished, and extractions happen under dental blocks for pain management.
The entire visit typically takes one to two hours. Modern veterinary anesthesia with proper monitoring carries a low mortality risk in healthy dogs, far lower than the historical perception and far lower than the accumulated risk of leaving the disease alone.
What Home Care Can and Cannot Do
Daily toothbrushing with an enzymatic pet toothpaste is the only home intervention that consistently slows plaque formation. Every-other-day brushing still shows meaningful benefit. The Veterinary Oral Health Council (VOHC) maintains a list of products (chews, diets, water additives, toothpastes) independently verified to reduce plaque or tartar. Looking for the VOHC seal is a faster filter than reading marketing copy.
A few things to avoid: antlers, bones, ice cubes, and hard nylon chews are a leading cause of fractured carnassial teeth. The test is whether the item flexes or dents under a thumbnail. If it does not, it is hard enough to break a tooth.
The Short Version
Bad breath is not normal. It is the most reliable early indicator of a disease that affects most adult dogs and that produces chronic pain most dogs will hide until treatment becomes more expensive and more complicated. Home care slows the process. A professional cleaning under anesthesia, including radiographs and proper scaling below the gumline, is the only intervention that can halt it. For dog owners across Osseo, Maple Grove, Brooklyn Park, and Champlin, practices such as Douglas Animal Hospital handle these visits routinely, and the right time to ask about one is usually earlier than owners think.